Unlike type 1 diabetes, insulin is still produced; however the issue arises with this insulin resistance and non-receptiveness of the body’s cells. In Australia, over 14% of the population lives with diabetes and it is thus a significant contributor to the burden of disease, with overall prevalence doubling since 1981. Additionally, diabetes is linked to an array of comorbidities including obesity, high blood pressure, cardiovascular diseases and some forms of cancers.
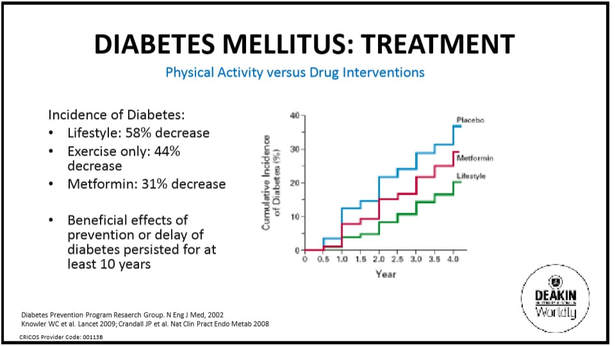
Type 2 diabetes is classified a lifestyle disease as it estimated that 90% of cases can be prevented through lifestyle modification, which includes participation in adequate physical activity as well as dietary changes. In terms of managing already diagnosed type 2 diabetes, the benefits that such lifestyle changes can have are significant. In fact, a study that tested the most effective method in reducing insulin resistance in type 2 diabetics found that lifestyle changes (combining both exercise and dietary changes) had the greatest improvement of 51%, followed by exercise only (44%) and finally, the benefits of metformin (31%) (Diabetes Prevention Program Research Group – The Lancet 2009). Metformin is the most common medication prescribed to type 2 diabetics, as it aims to improve glucose uptake into peripheral cells via improving insulin-sensitivity, whilst aiming to lower blood sugar levels via decreasing production of insulin in the liver. Despite this, the improvement in insulin sensitivity resulting from lifestyle changes alone proved to be 20% higher!
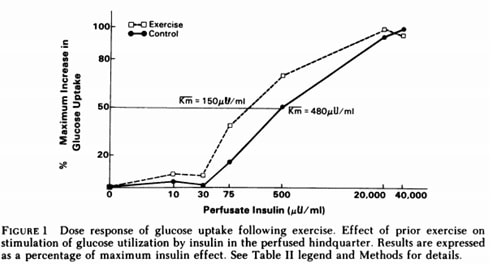
Studies have been conducted in order to determine the most effective type of exercise for treating type 2 diabetes, and it has been determined that using both aerobic exercise and resistance training in synergy provides the greatest results. A study conducted by Richter et al. found that insulin-stimulated glucose uptake in skeletal muscle was enhanced following an acute bout of aerobic exercise, the effects of which have been found to last for up to 48 hours (Richter et al. 1982). Furthermore, such exercise was found to produce a 31% reduction in hyperglycaemia in the 24 hours following exercise, as exercise lowered blood glucose concentrations by an average of 0.9 mmol/l (Van Dijk et al. 2013). Aerobic training in the form of cycling over a 10 week period produced similar results, with glucose uptake improvements in both type 2 diabetic and healthy subjects (Dela et al. 2006).
Alternatively, chronic resistance training has also been found to improve glucose uptake, while it also offers benefits in strength and functional capacity improvements (Holten et al. 2004). The basis for this surrounds the fact that skeletal muscle accounts for 80% of total insulin stimulated glucose uptake due to its large mass (30-40% of body mass) and high oxidative capacity, as the primary fuel skeletal muscle utilises are carbohydrates, or glucose (Defronzo & Tripathy 2009). Maintaining muscle mass is extremely important as a 50% decline in insulin-stimulated glucose uptake has been found in type 2 diabetics when compared to healthy subjects (ref p. 7 same as above). Essentially, skeletal muscle is the primary ‘up-taker’ of glucose, and therefore increasing skeletal muscle mass allows for more sites to take up glucose, thus reducing blood sugar levels significantly!
At Inspire Fitness for Wellbeing we conduct exercise classes for people with Type 2 Diabetes under the supervision of an Accredited Exercise Physiologist . These sessions have been running for 4 weeks and have so far proven very successful. Our classes incorporate a mix of cardiovascular and resistance training to suit each individual participating as per recommended guidelines. They involve a handful of type 2 diabetic clients training together for one hour with supervision of an Exercise Physiologist either once or twice a week. Furthermore, clients are educated on lifestyle changes that can be made, as well as some of the information throughout this blog, in order to motivate and inspire positive change both inside and outside the class! Here are some of the comments made by clients so far:
Shane (Monday’s class): “I really hope the group stays together because I’m really enjoying it and would struggle to do it alone.”
Ishva (Monday’s class): “I saw my GP and my blood glucose has dropped so much that she may be taking me off my insulin medication”
If you are a type 2 diabetic and think some of these lifestyle changes are essential for you please contact us on 9857 3007 to enquire about joining one of our classes, we’d love to have you!
References:
DeFronzo, R.A. and Tripathy, D., 2009. Skeletal muscle insulin resistance is the primary defect in type 2 diabetes. Diabetes care, 32(suppl 2), pp.S157-S163.
Diabetes Prevention Program Research Group, 2009. 10-year follow-up of diabetes incidence and weight loss in the Diabetes Prevention Program Outcomes Study. The Lancet, 374(9702), pp.1677-1686.
Holten, M.K., Zacho, M., Gaster, M., Juel, C., Wojtaszewski, J.F. and Dela, F., 2004. Strength training increases insulin-mediated glucose uptake, GLUT4 content, and insulin signaling in skeletal muscle in patients with type 2 diabetes. Diabetes, 53(2), pp.294-305.
Rabøl, R., Boushel, R. and Dela, F., 2006. Mitochondrial oxidative function and type 2 diabetes. Applied Physiology, Nutrition, and Metabolism, 31(6), pp.675-683.
Richter, E.A., Garetto, L.P., Goodman, M.N. and Ruderman, N.B., 1982. Muscle glucose metabolism following exercise in the rat: increased sensitivity to insulin. The Journal of clinical investigation, 69(4), pp.785-793.
Van Dijk, J.W., Venema, M., Van Mechelen, W., Stehouwer, C.D., Hartgens, F. and Van Loon, L.J., 2013. Effect of moderate-intensity exercise versus activities of daily living on 24-hour blood glucose homeostasis in male patients with type 2 diabetes. Diabetes care, p.DC_122620.

 RSS Feed
RSS Feed
